Prevention and Treatment of Urinary Incontinence
A middle-aged woman's struggle with not being able to talk to others
Why you may need the treatment for urinary incontinence
It's easy to think of urinary incontinence as just a condition where urine leaks, leading to the question, "Is treatment really necessary?" However, urinary incontinence can cause significant disruptions to daily life. The uncertainty of when and how urine might leak can lead to feelings of anxiety and excessive stress.
Experienced by about 40% of women, urinary incontinence is a condition in which urine leaks from the bladder against one's will, causing problems, and is more common in middle-aged women than in men.
Urinary incontinence is a treatable condition, so it's important to seek appropriate treatment with the help of a healthcare provider, as the discomfort and impact on quality of life can be significant if it's treated as a normal part of aging, ashamed or ignored.
- 1Accurate diagnosis and treatment: Accurately identifying the type of incontinence (stress, urge, etc.) and cause is important for proper treatment planning.
- 2Discover potential risks: Other health problems (cystitis, enlarged prostate) associated with urinary incontinence can be detected and treated. In rare cases, urinary incontinence can also be a sign of spinal cord disease.
- 3Improved quality of life: Urinary incontinence can cause embarrassment, difficulty with daily activities, and decreased self-esteem, so proper treatment can significantly improve quality of life.
- 4Help prevent complications: Untreated urge incontinence, especially in cases of neurological disease, can lead to serious complications, including increased bladder pressure, kidney inflammation, and kidney failure.
- 5Personalized care: Considering your condition, medical history, lifestyle, and more, we can suggest the most appropriate treatment for you.
- 6The good thing about early diagnosis: The earlier incontinence is treated, the better the outcome.
- 7Identify comorbidities: Other health issues related to urinary incontinence (e.g., cystitis, prostate enlargement) can be detected and treated.

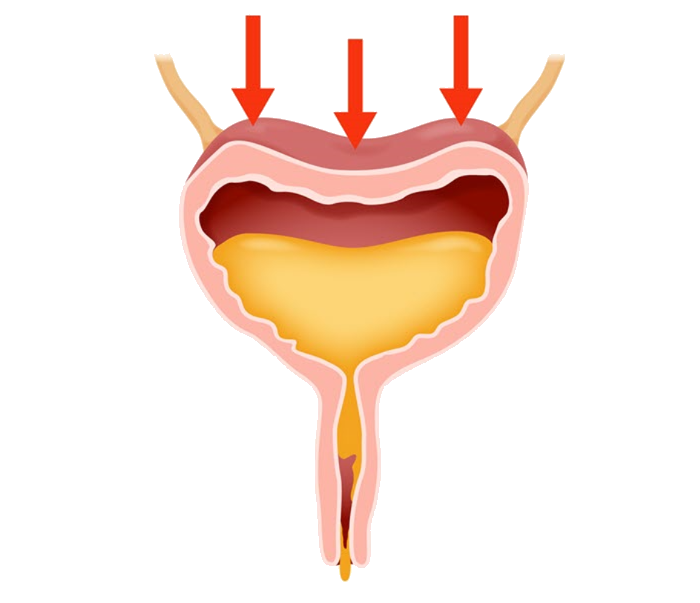
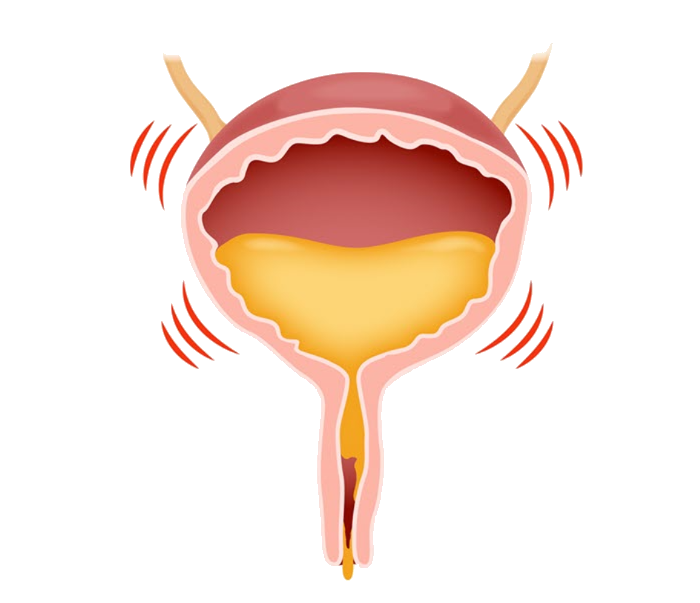
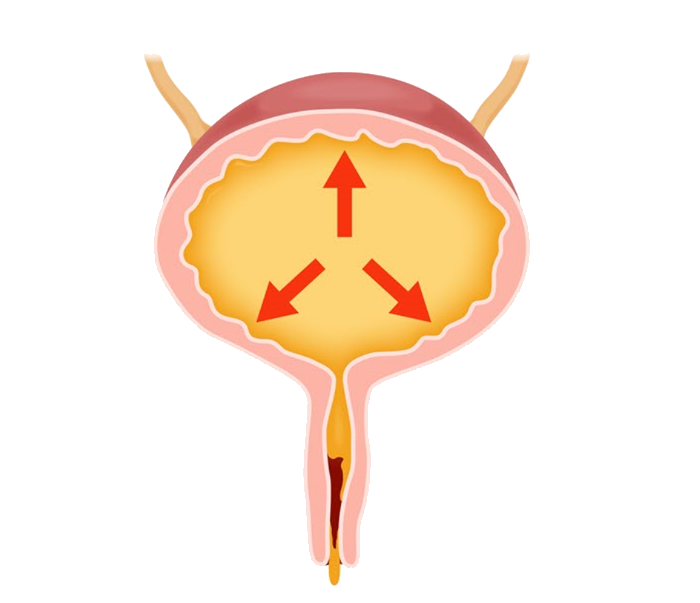
Types of Urinary Incontinence

How to self-test for urinary incontinence
- 1Urine leaks out when you cough or sneeze.
- 2I feel pain in my lower abdomen when I urinate.
- 3My stomach hurts when I urinate.
- 4On your way to the bathroom, you can't hold it in and urine leaks out.
- 5You urinate in your sleep more than 2 times a night.
- 6I don't feel better after urinating.
- 7I've leaked urine during sexual intercourse.
Causes of urinary incontinence in middle-aged women
Shorter urethra compared to men
Elevated abdominal pressure
Pregnancy and childbirth effects
Medications and stress
Congenital defect
Pelvic muscle relaxation due to aging
Menopause and hormonal changes
Eating foods that irritate the bladder
How to treat urinary incontinence
Your doctor will decide how to treat you after consulting with you, taking into account the type of incontinence, severity, and your condition.
For combined incontinence, surgical treatment for overflow incontinence may be combined with medication for urge incontinence
▪️ Midurethral sling surgery: A method of supporting the urethra with an artificial tape, used primarily for stress urinary incontinence in women.
▪️ Botulism toxin injections: Surgery to inject botulism toxin into the bladder to inhibit overcontraction of the detrusor muscle, used for urge incontinence
▪️ Sacral Nerve Modulation: A treatment that stimulates the sacral nerve, which connects the anus and rectum, to relieve tension in the bladder and pelvic muscles to control urination.
▪️ Bladder volume augmentation: Treatments to improve urination function by increasing the volume of the bladder that stores urine
▪️ Artificial Urethral Sphincter Insertion: A treatment used for urinary incontinence after prostate surgery in men, effective for patients with difficulty controlling urination
▪️ Pelvic floor exercises (Kegel exercises): Exercises to help treat urinary incontinence by strengthening the sphincter, repeating each exercise 10 times at least 8 to 10 times a day.
▪️ Biofeedback: How to exercise with a monitor that detects pelvic floor contractions
▪️ Electrostimulation therapy: Stimulates the pelvic floor muscles with a mild electric current to strengthen and contract the muscles to improve urinary control.
▪️ Extracorporeal magnetic innervation: Improves urination function by stimulating muscles and nerves with magnetic fields
▪️ Behavioral therapy: Train your bladder by holding and collecting urine while controlling your fluid intake.
▪️ : Medication treatment: Use of anticholinergics or beta3 receptor agonists for urgency incontinence, and no medication for urge incontinence in women
Kegel exercises helpful for urinary incontinence
Kegel exercises were first developed by American gynecologist Arnold Kegel to exercise the pelvic floor muscles. They were developed to treat female urinary incontinence by strengthening the pelvic muscles that have been stretched by childbirth or aging, and are known in the medical community as "pelvic floor exercises."
Kegel exercises have become popular as a sexual intercourseual enhancement exercise, as they have been found to be effective not only for urinary incontinence, but also for promoting sexual intercourseual sensation. Our muscles get weaker with each passing day, and as they get weaker, our body's ability to contract and relax deteriorates, so doing Kegel exercises every day is a great way to help prevent incontinence.
- For maximum effectiveness, it's best to do it every day, morning and evening.
- We recommend doing 10 repetitions of each movement at least 8 to 10 times a day.
- Kegel exercises may seem tedious at first, but with practice, you'll be able to do them in a short amount of time.